

Since joining the hospital in 2015, Dr. Webb has successfully led efforts to improve patient outcomes, enhance the patient experience and grow revenues. Prior to joining Nashville General Hospital, Dr. Webb served as chief operating officer for Common Table Health Alliance in Memphis, Tennessee. As a former chief executive operating officer for Methodist Le Bonheur South Hospital in Memphis, Tennessee, he held additional chief executive roles for Healthcare Services of America at Coastal Carolina Hospital and Northwest Mississippi Regional Medical Center. Dr. Webb concluded his tenure at NGH in early 2025 and continues his work in healthcare leadership and advocacy.
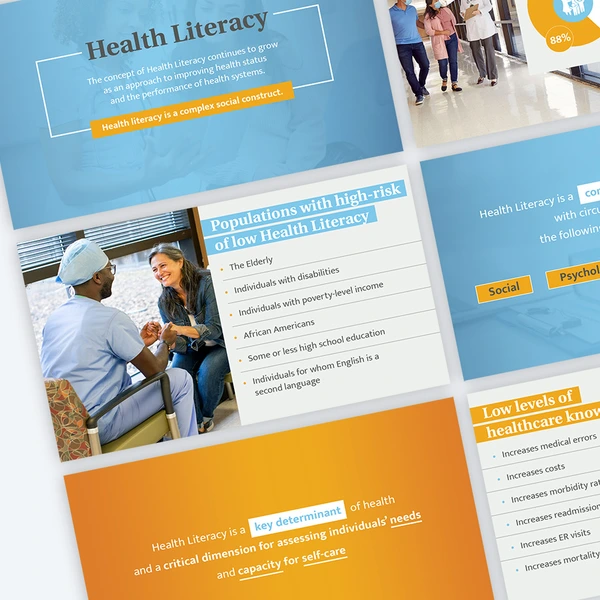
One Neighbor at a Time: Dr. Joseph Webb's evidence-based approach for Nashville General Hospital to address Health Literacy.
The concept of Health Literacy continues to grow as an approach to improving health status and the performance of health systems.

Dr. Webb is board certified in Healthcare Management and is a Fellow in the American College of Healthcare Executives. Dr. Webb earned a Doctorate of Science in Health Services Administration and Master of Science in Hospital and Health Services Administration from the University of Alabama at Birmingham. He also holds a Master of Science in Health and Physical Education and a Bachelor of Science from Tennessee State University.
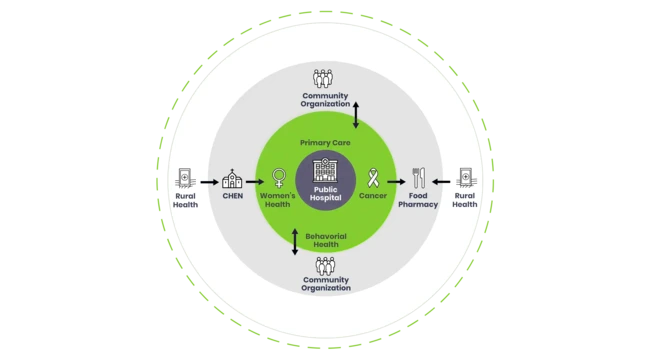
Dr. Webb is the author of the Health Equity Model (WHEM), a “hub and spoke” healthcare delivery process founded on the principles of evidence-based management. EBM is the “systematic application of the best available evidence to management decision-making, aimed at improving the performance of healthcare organizations.” As part of this approach, WHEM leverages the Patient Centered Medical Home (PCMH) and Chronic Care Management model to bring holistic, proactive healthcare and well-care to the individual where they live—in the community. The WHEM model addresses health literacy, creates referrals to care through community organizations and ensures continuity of care.

We don’t have an access issue with healthcare, we have a health literacy and care coordination problem that traditional healthcare is not incentivized to solve. We’ve solved it in Nashville through our hub and spoke model, including a community-based strategy; with the right leadership, this can be done in any metropolitan city in America.